Your neck usually doesn’t get much attention, not until something goes wrong, that is. But this small, sturdy part of your body (also known as your cervical spine) does a lot more than you think. It holds your head up all day, lets you turn and look around, and quietly protects the vital nerves that run between your brain and the rest of your body. With that kind of workload, it’s no surprise your neck can get into some trouble from time to time. In this article, we’ll go over the most common neck injuries and what you can do if you ever find yourself dealing with one.
First, we should go over some anatomy.
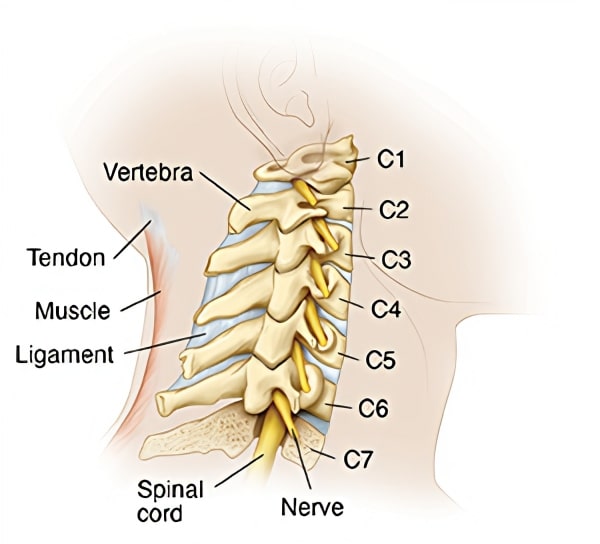
Your neck is made up of 7 stacked bones, called vertebrae, labeled C1 through C7. Think of them kind of like a carefully balanced Jenga tower. Between each of those wooden pieces are your discs, which act as shock absorbers and help protect your spine.
Your neck isn’t just bones though, it’s a whole team effort. You’ve got muscles, ligaments, tendons, and nerves all working together to keep your neck stable and moving the way it should. And running right through the center of it all is your spinal cord, which sends messages between your brain and the rest of your body. That means every move you make or sensation you feel relies on those signals traveling smoothly up and down your spine.
Now that you know the basics, it’s time to take a look at some muscle and tissue injuries.
Muscles & Tissue
Usually when people talk about neck pain, they blame the big obvious stuff, like bones or discs. But the real troublemakers are the muscles and soft tissue around them. After all, they’re what gives your neck its flexibility and strength. They’re also the first to get irritated when they’re stressed or overworked.
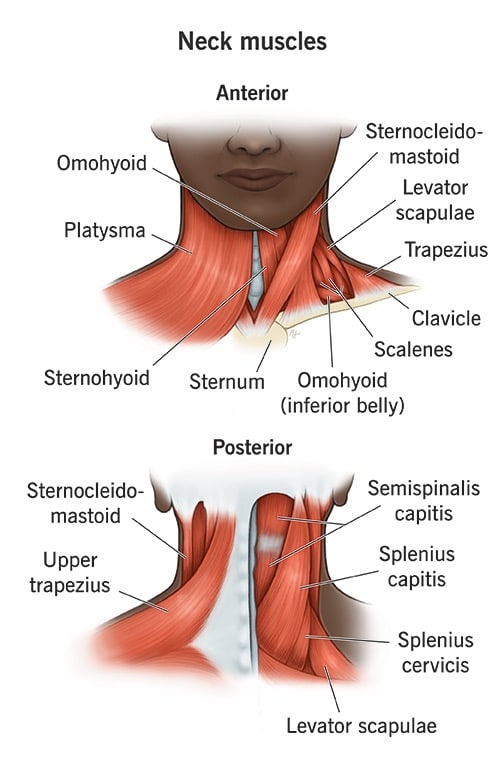
There are roughly 20 to 30 muscles in your neck. Some help with the more noticeable motions (like turning your head side to side), while others work behind the scenes to make small tiny adjustments you don’t even think about. These muscles attach themselves to your bones through strong, flexible cords called tendons. Add in your nerves, which are constantly sending messages between your body and your brain, all working together so you can make smooth, controlled movements.
Cervical Strain
With so many moving parts, it’s not really surprising when an injury pops up. One of the most common is a cervical strain. Basically, it’s when a muscle or tendon in your neck gets overstretched or slightly torn. Sometimes neck strains are called a “pulled muscle,” which may not sound super serious, but depending on where it happens and how severe it is, it can be incredibly painful and restrictive.
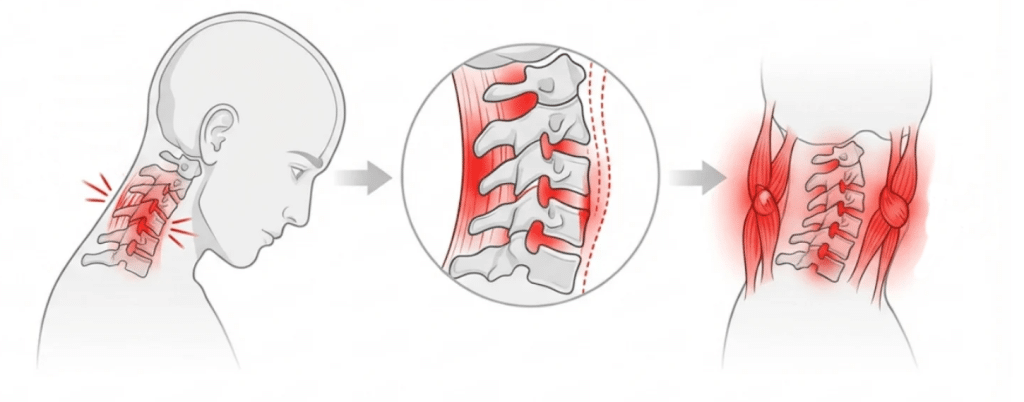
A quick thing to keep in mind is that neck strains are different from neck sprains. Strains involve muscles and tendons whereas sprains affect your ligaments (but we’ll get to that a bit later on in this article.)
Symptoms
Neck sprains are broken down into 3 different categories based on how much damage there is.
- Grade 1 strains are the most mild. It usually means a few muscle fibers got overstretched or torn. You might feel some tightness and soreness, but your strength and movement should remain normal for the most part.
- Grade 2 strains are more moderate. With these strains, there’s a larger tear through your muscles, so the pain is more noticeable. You might feel weaker, your movement can be limited, and it may take a bit longer to recover, but it’s still very manageable.
- Grade 3 strains are the most severe. These involve a complete tear of your muscle, and the pain can be so intense that it’s practically paralyzing. These aren’t as common as the other 2, but when they do happen, it’s usually alongside some serious damage to your spine.
Most neck strains are on the mild to moderate side and eventually heal with time, but that doesn’t mean they’re easy to live with. Even minor ones can mess with your sleep and make everyday tasks way harder than they should be.
Different Kinds Of Discomfort
One of the first things you’ll notice when you have a cervical strain is pain. It usually sticks to the back of your neck, but it can spread to your shoulders and up toward the base of your head too. For most people, it starts as a dull, deep ache, then shifts into more of a throbbing sensation later on at night. It might even get to the point where a simple movement, like reaching for something, can trigger a sharp jolt of pain and catch you off guard.
Stiffness is another big one. Your neck might feel tight, like it’s stuck in place and can’t move. When this happens, your muscles have tightened up either to protect itself or from all the swelling going on. It’s also not uncommon to get some numbness or tingling down into your arms and possibly even your hands.
Causes
As for the reason behind your neck strain, there are a few different things that could be to blame. In most cases, it’s because of poor posture. You’d be shocked at how quickly your muscles and tendons can get overstretched when you’re hunched forward or sitting at an awkward angle. Even something as simple as sleeping in a weird position can strain your neck. And now that phones and tablets seem to be glued to everyone’s hands, posture problems are bigger than ever.
Lifting something that’s way too heavy is another way to strain your neck. Most people think of back injuries in this type of situation, but you can easily overexert your neck here too. There’s only so much that your muscles and tendons can handle.
Then there’s repetition. Whether it’s for your job or just a hobby, doing the same motions over and over can slowly wear down your neck. On the flip side of things, jumping into an intense or unfamiliar activity can be just as bad if your body isn’t used to it.
Diagnosing
Most neck strains never actually get officially diagnosed. That’s because a lot of them usually calm down on their own within a few days or so. But if your symptoms persist or get worse, then it’s a good idea to go see your doctor.
They’ll start by getting your medical history and then ask about any recent activities or habits that may have irritated your neck. After that, your doctor will feel around your neck for any tender spots and watch as you move your head in different directions. They’ll also do a few tests, especially if you have pain or tingling that radiates down past your elbow.
In some severe cases, a physical exam might not be enough. That’s when they’ll order imaging, like X-rays or an MRI, to confirm their diagnosis. These scans will also help rule out any other injuries that can look and feel similar to a strain.
Treatment
When it comes to neck strains, the right treatment really makes a huge difference. It’ll lower your pain and discomfort, speed up your recovery, and get you back to your normal routine quicker too. You just have to find the combination that works best for your body.
As soon as you first notice any pain, you should step back and take it easy for a while. Ideally, this means avoiding any strenuous or irritating activities or tasks. For all the things you can’t avoid, try changing the way you do them so they’re easier on your neck. You want to give your muscles and tendons a chance to calm down and start healing. Make sure you don’t push through the pain because that’ll only make your recovery longer.
Now, ‘taking it easy’ doesn’t mean doing absolutely nothing at all. Gentle, controlled movement is going to be key here, but sometimes it’s difficult to know exactly what that looks like. That’s where physical therapy comes in.
Physical Therapy
Physical therapy is so effective because it looks at the bigger picture. Instead of just treating your symptoms, the therapist works to find the root cause of your strain. They’ll create a personalized plan that targets your neck and the surrounding areas. They’ll guide you through specific exercises and stretches designed to reduce pain, restore movement, and support healing, all without aggravating your injury.
Early on, you’ll focus on proper form and control of your movements. As your neck improves, you’ll learn new, more challenging exercises. The ultimate goal isn’t to be in physical therapy forever, it’s about independence. Once you graduate from PT, you’ll be able to continue your exercise program at home on your own. These exercises will become your tools for success long term, but you can also do them anytime you have a flare up.
Cervical Radiculopathy
Next up is cervical radiculopathy. Cervical radiculopathy, better known as a pinched nerve, happens when the nerves in your neck get compressed (or pinched.) The nerves in question stem out of your cervical spine and travel down into your shoulders, arms, and hands. So, when something is off, you can usually feel it beyond just your neck.
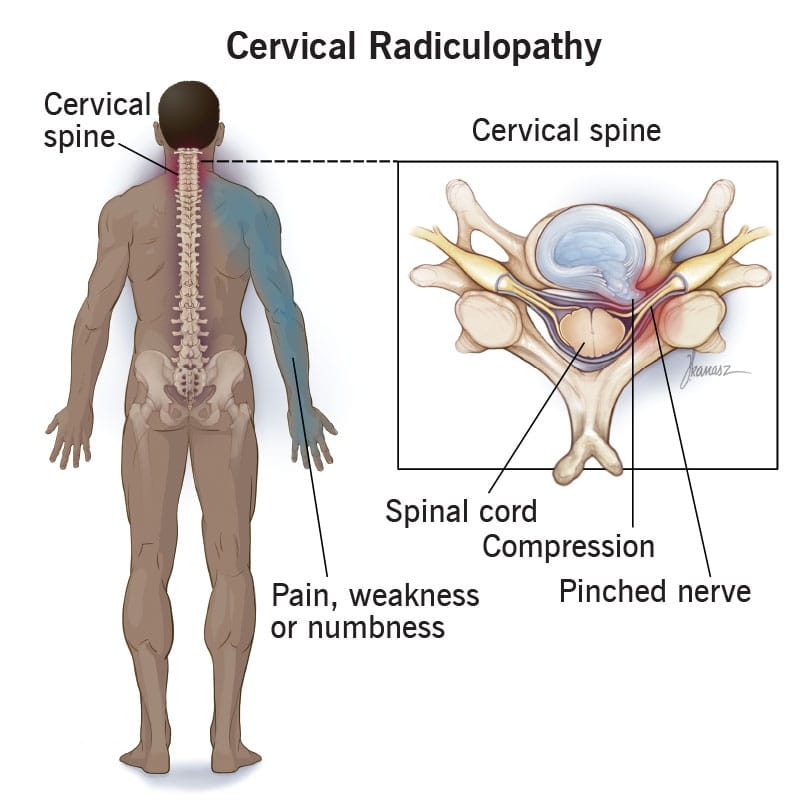
When one of your nerves gets compressed or inflamed, it can’t send or receive signals from your brain like it’s supposed to. This kind of breakdown in communication is what’s known as a neurological dysfunction. So, if you have cervical radiculopathy, it’s pretty easy to recognize.
Symptoms
Cervical radiculopathy is kind of unique because instead of your symptoms just staying in your neck, they can actually travel along the path of your nerves. That means you could have pain in your neck, shoulders, arms, and hands all at the same time. You might even get some numbness and tingling too.
Typically, symptoms stick to one side of the body at a time, but in some cases it can affect both. The intensity depends on how irritated your nerves are. They’ll range anywhere from mild and a bit annoying to super intense and restrictive.
Unlike strains, the type of symptoms that come with a pinched nerve tend to feel sharper, more electric, almost burning. They also usually follow a very specific pattern down your arm instead of just showing up randomly. Your nerves are kind of like a cable, sending glitchy signals while it travels along its route. You can easily track it and see where it’s going to go next.
Causes
Anyone can get cervical radiculopathy, but it’s way more common the older you get.
If you’re under 50, it’s usually due to a herniated or bulging disc in your neck. That’s when the outer layer of your disc starts to weaken and eventually cracks. Once that happens, the jelly material inside your disc can “leak” out and press against your nerve, causing those classic radiculopathy symptoms.
Now, if you’re in your 50’s or 60’s, then it’s more likely that degenerative disc changes are to blame. This is the age where your discs start to lose their height and flexibility, making it easier for your nerves to get pinched.
By your 70’s, you’re likely very familiar with arthritis related changes to your body, so it’s probably not surprising to hear that it leads to radiculopathy too.
Diagnosing
If you think you might have a pinched nerve, you’ll want to get it checked out sooner rather than later. Your doctor will be able to examine your neck and all the areas around it. They’ll also assess your reflexes, look for muscle weakness, and see if you notice any different sensations in your arms or hands.
It can be a little tricky to diagnose cervical radiculopathy because there’s other neurological conditions that cause similar symptoms. So if your doctor isn’t 100% sure, they may send you to get an MRI or X-ray to rule out other injuries and help confirm what’s going on.
Treatment
Most people with pinched nerves improve on their own after a few months. But recovery is usually much more successful with the help of physical therapy. Overall, it’ll be a combination of time, managing your symptoms, and being smart with your movements.
Your therapist will focus on building strength in your neck, increasing flexibility, and calming down those irritated nerves. In the beginning, you’ll learn exercises that work on your range of motion without triggering flare ups. Then as things improve, you’ll gradually move on to strengthening and conditioning exercises for your spine. The PT will also teach you how to keep better posture, small changes you can make around the house, and safer ways to do any risky work or home activities.
One thing to keep in mind is cervical radiculopathy never truly goes away. In fact, more than 33% of people end up having their symptoms come back at some point. The upside is you won’t be starting from scratch, you already have the tools and exercise program you need to manage it and get back on track again.
Myofascial Pain Syndrome
This next injury we’re going to cover is called myofascial pain syndrome. The name might sound a bit confusing, but it’s actually pretty simple. Basically, myofascial pain syndrome is a chronic pain condition that comes from swelling in your neck muscles and fascia.
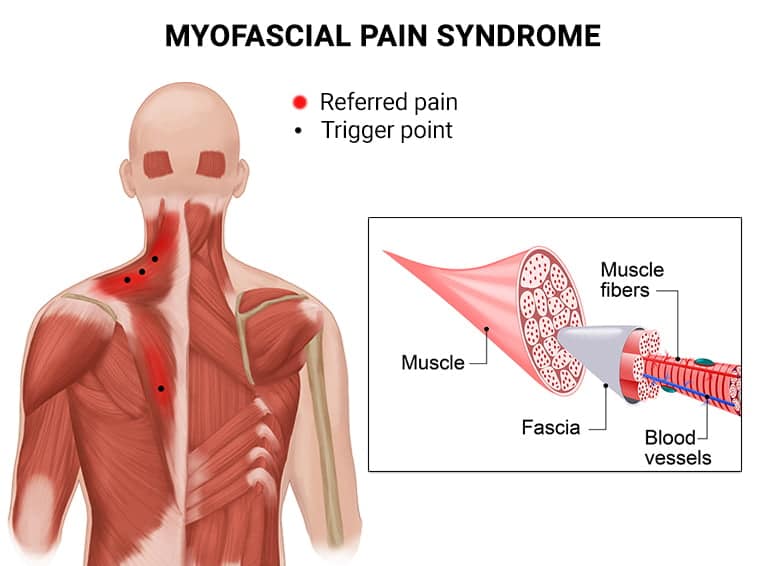
If you haven’t heard of “fascia” before, it’s just the fancy term for the thin connective tissue that wraps around your muscles. Think of your body like an orange. The peel is your skin, the fruit on the inside is your muscles, and that weird stringy white webbing around each orange slice is your fascia. It helps everything glide smoothly whenever you move.
Symptoms
Odds are, you haven’t heard much (if anything) about myofascial pain syndrome, but it’s a lot more common than you realize. Nearly 85% of people experience it at some point in their life. The tricky part is that it doesn’t feel the same for everyone.
Some get a sudden, intense pain that shows up out of nowhere. For others, it’s more of a dull, nagging ache that lingers in the background and slowly wears you down as the day goes on. Most people say it’s like a persistent throbbing type deep in the muscle.
It’s not uncommon to get physical trigger points, like small knots or nodules that hurt when you press on them. You might also notice that your muscles feel tender, tight, and even weaker than normal. If it becomes difficult to move your neck and shoulders, then that’s a sign that things are getting worse. All of your symptoms will start to get more noticeable (and more sensitive) the longer it’s left untreated.
Causes
Myofascial pain syndrome can be frustrating because there’s no one single clear cause. Usually, it seems to develop from a mix of things, like physical stress, muscle imbalances, and other underlying health issues.
There are also some risk factors that don’t necessarily cause myofascial pain syndrome directly, but can increase your odds of developing it. Sitting too much is a big one because your muscles start to get stiff and weak. Stress, especially the kind you carry in your shoulders, can make you tense up without even realizing it. And once your neck muscles aren’t pulling their weight, other muscles are forced to work overtime in order to pick up the slack (which only adds to the strain.)
Diagnosing
Myofascial pain syndrome is often overlooked. Not because it isn’t real, it just looks a lot like some other kinds of conditions. Anytime symptoms involving your nerves or tendons overlap, it’s easy to dismiss or mislabel them.
Getting a proper diagnosis starts with a physical exam. Your doctor will take a hands-on approach and feel around your muscles and look for any trigger points in your neck. When they press down, the pain might stay right in that spot or travel a bit.
Since there aren’t any visible signs like redness or swelling, doctors usually do tests that rule out other conditions. They’ll want to know how your pain feels, what types of things make it worse, and if your symptoms change throughout the day.
Treatment
Luckily, this is a condition that’s very treatable, especially if you catch it early. The key is recognizing the symptoms sooner rather than later. And you’ll want to start treatment before you get any trigger points and your pain becomes unmanageable.
Most doctors recommend seeing a physical therapist because of their expertise in treating the specific pattern, severity, and location of myofascial pain. They focus on loosening your tight muscles, strengthening the weak ones, and helping everything move more efficiently. They’ll also create an exercise program to do at home so you can continue progressing even on the days you don’t have therapy.
Herniated Disc
The last soft tissue injury we’ll cover is a herniated disc. When you have a herniated disc, it means that one of the discs in your spine developed a crack and the gel inside pushes out. Once that cushiony material escapes, it can press on your spinal cord or nearby nerves.
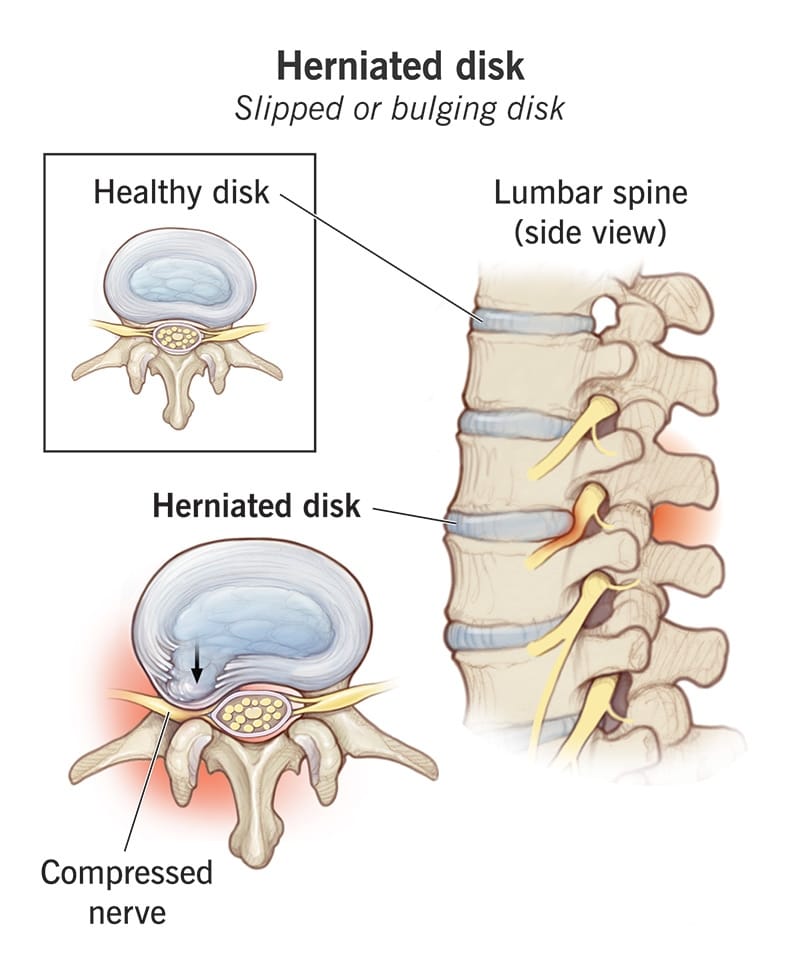
As you know, you’ve got 7 bones in your neck stacked on top of each other, with discs in between that act as shock absorbers. Each disc has two main parts: a soft jelly center (the nucleus pulposus) and the tough outer layer (the annulus fibrosus.) Together, they give your neck stability and allow you to move it freely.
Symptoms
Most neck herniations bulge to one side or the other, rather than straight back. That means you’ll likely get the majority of your symptoms on just the right or left side of your body, depending on which nerve is involved. And it’s usually the discs between C5-C6 and C6-C7 that are affected since they handle the most movement and stress.
Symptoms can be surprisingly unpredictable. Some people feel a clear, consistent pain, while others barely notice anything at all. Once the symptoms do show up though, they can vary in how they feel, how long they last, and where they travel.
When it comes to pain, it can feel like a dull ache or something sharper, almost electric. It might stay in your neck or it could go down into your shoulders and arms as well. Some people also get tingling or numbness along with it. Usually the symptoms come in waves, following a pattern that starts with a flare up then slowly fades away. Certain movements and activities can make them worse too.
Causes
The two biggest causes of a herniated disc is degeneration and trauma. With degeneration, your discs naturally dry up over time, making them less flexible and more prone to cracking. Trauma, on the other hand, typically involves a fall, car accident, or some type of sudden direct blow to your neck, which causes your disc to herniate.
Your risk of developing a herniated cervical disc increases as you get older. In fact, most people get them between 30 to 50 years old. And they don’t happen overnight either, it’s a gradual thing.
Diagnosing
Diagnosing a herniated disc takes a full picture rather than just relying on a single test. Your doctor will start with a medical history, asking about past injuries and if you have had any prior neck or back pain. They’ll also ask about your current symptoms and when you first noticed them.
Next comes the physical exam. They’ll check to see if there’s any swelling or tenderness in your neck, test your range of motion, and evaluate your strength, reflexes, and feeling through your arms and hands. All of these things are essentially looking for signs of nerve involvement.
Your doctor may order some imaging tests if they’re still not 100% sure in their diagnosis. If it shows a herniated disc, it will fall into 1 of 2 categories: contained or uncontained. Contained herniations mean the bulge goes into the small tears of your disc, but still stays within the disc itself. Uncontained means the inside material breaks through the outer layer and starts to leak. In both situations, the bulge can press against your nerves or spinal cord, which is what causes your symptoms.
Treatment
In most cases, you can manage the symptoms of a disc herniation without surgery. At first, you’ll want to take things slow and rest your neck so it isn’t so sensitive. You don’t want to be completely inactive though, just avoid positions and activities that trigger your symptoms.
Once things calm down, your next step will be starting physical therapy. The beauty of PT is that it focuses on reducing the stress on your spine and strengthening the muscles that support your neck.
Simple exercises, like chin tucks, can go a long way with improving your posture and keeping your head and neck in alignment. When your head is in a neutral position (meaning your ears are directly above your shoulders), there’s less stress on your cervical spine and discs. Strong, balanced muscles help make that alignment possible and takes the strain off of your neck.
Your physical therapist will also recommend modifying some of your daily habits and activities, especially the riskier ones. Small changes, like how you move, sit, lift, and even sleep, will make a huge difference in how quickly (and how well) your neck recovers.
Ligaments
Now, let’s talk about ligaments. Ligaments are tough bands of tissue that connect your bones to each other. They keep things stable, restrict excessive movements, and support your spine.
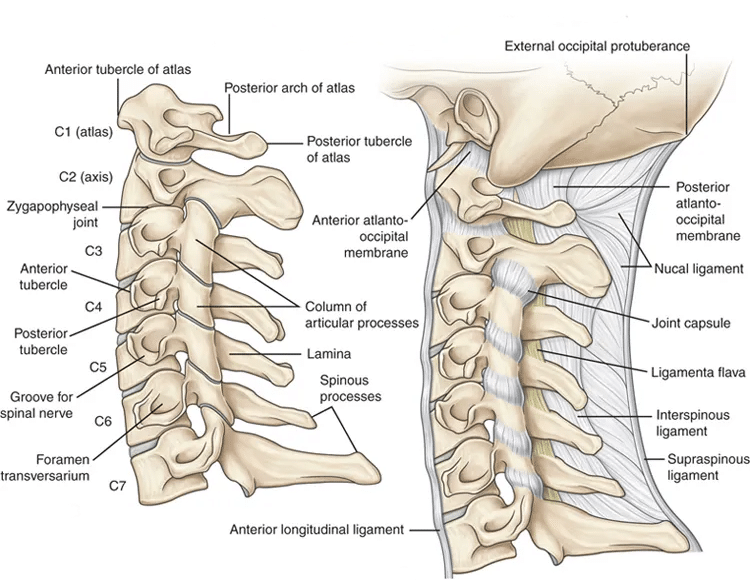
Your ligaments specialize in control. When you’re moving your neck, they help guide everything. And when you’re not, they help prevent injuries, especially from sudden and unexpected movements. Basically, healthy ligaments provide just enough restraint without completely changing your neck’s natural motion.
Neck Sprain
The first ligament injury we’re going to cover is a neck sprain. And yes, neck sprains are different from neck strains. Strains affect muscles and tendons, while sprains involve damage to your ligaments.
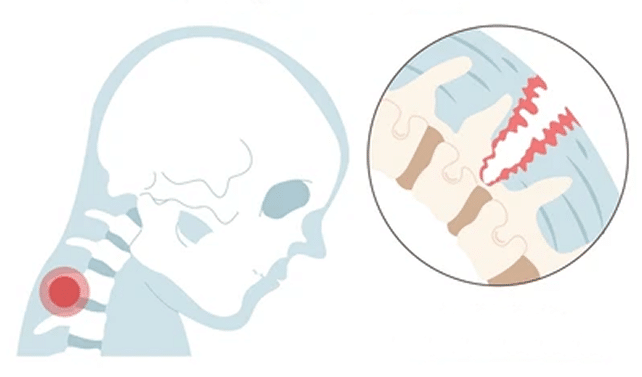
Remember, you’ve got 33 vertebrae in your spine, all held together by ligaments. When it comes to your neck, there are 5 main ligaments: anterior longitudinal ligament (ALL), posterior longitudinal ligament (PLL), supraspinous ligament, interspinous ligament, and the ligamentum flavum. If one (or more) of these ligaments gets injured, then even the tiniest movements like turning your head can become super painful.
Symptoms
Like strains, sprains are graded on from 1 to 3 depending on their severity, and each have their own symptoms.
- Grade 1 sprains have mild stretching or partial tearing. You’ll likely feel some minor pain and a bit of instability.
- Grade 2 sprains involve a more significant tear (over 50% of the ligament.) Because of this, your symptoms will be a lot more noticeable.
- Grade 3 sprains are the most severe because it means you’ve completely torn through your ligament.
With serious sprains, doctors will want to see whether your ligament has pulled apart. If the fibers are still in their normal spots, then it’s considered non-retracted. But if they’ve separated, it’s a retracted tear and you’ll likely need surgery.
Symptoms may come and go or change intensity throughout your day. For most people, they notice pain in the back of their neck and sometimes into their upper shoulder blade area too. It usually gets worse a day or two after their injury or when they start moving again.
Besides pain, you might have to deal with headaches, muscle spasms, and neck stiffness. It’ll also be difficult to turn or tilt your head. In some cases, numbness and a tingling sensation can travel down into your arms and hands. And like many neck injuries, your symptoms may start off fairly light and gradually get worse over time.
Causes
Neck sprains are usually caused by overuse or from some kind of injury.
For instance, if you like to carry your bag or heavy purse on the same shoulder over and over, that can slowly strain your ligaments. Car accidents or injuries involving whiplash can do it as well. And sometimes something as simple as sleeping in an awkward position or on a pillow that’s too high, too low, or not supportive enough is all it takes.
Diagnosing
The best way to diagnose neck sprains is with a physical exam. Your doctor will ask about your pain levels, check your strength, range of motion, and look for any tender spots. They’ll also do some functional tests to figure out the grade and severity of your sprain.
In some cases, your doctor may want to do some imaging. Things like X-rays and MRI scans can help rule out other conditions, especially ones with similar symptoms. These also help make sure there’s nothing else contributing to your pain.
Treatment
There’s no one-size-fits-all solution for neck sprains (which is actually a good thing.) Your treatment should be something that matches your specific injury. And physical therapy plays a huge role in these situations.
At PT, your physical therapist will focus on managing your pain while gradually restoring movement back into your neck. They’ll teach you stretches and exercises designed to strengthen your muscles and improve flexibility. The goal isn’t just feeling better in the current moment, but to help you get back to your daily routine and lower your chances of dealing with this same issue in the future.
Text Neck
This next one has gotten a lot of attention over the years. It’s called text neck, and it’s a type of injury caused by spending long periods looking down at your phone, tablet, or other handheld device. Tilting your head forward, even just a little bit, may seem harmless, but over time it can change the natural curve of your neck and put extra strain on the ligaments that support it.
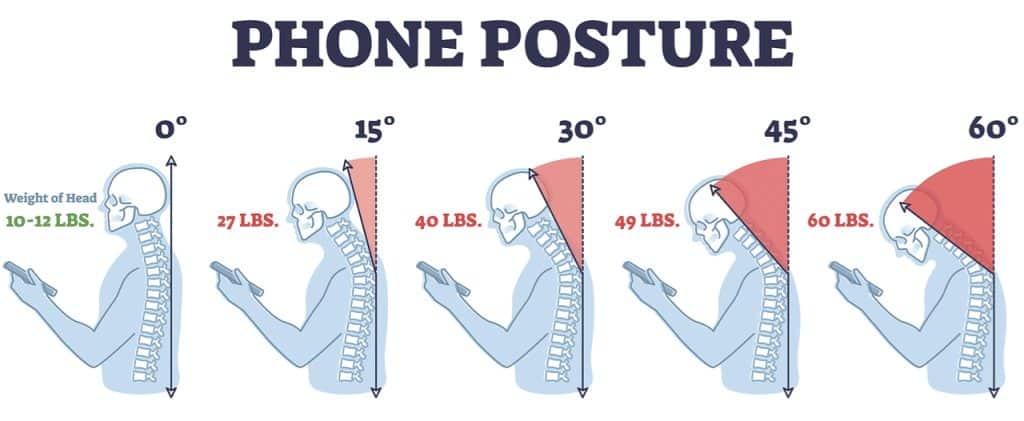
Now, here’s the real eye opening part. The more your head tips forward, the heavier it feels to your neck. At just a 15° tilt, you’re adding 27lbs of force! A 30° tilt jumps to 40lbs of pressure, and 60° adds an extra 20lbs, putting you at a whopping 60lbs of force! That’s like carrying an 8 year old child on your neck all day.
Symptoms
Text neck doesn’t just appear overnight. It gradually builds up as you keep tilting your head forward and stressing your neck. So what starts out as just a little discomfort can quickly turn into chronic pain if you’re not careful.
Usually the first thing people notice is an achy tightness in their neck muscles. This is your body working overtime to hold your head in that tilted position. You might also get headaches that shoot up the back of your neck too. All of these things will be even more noticeable the longer you look down at your phone or tablet.
Even though it’s called text neck, your symptoms don’t always stay in your neck. A lot of people end up getting pain in their shoulder blades and upper back area. If you have a more severe case of text next, then your nerves might be involved too, which often leads to numbness or tingling down into your arms and hands. When this happens, it can cause weakness, fatigue, and even trouble concentrating.
Causes
Like the name suggests, text neck comes from repeatedly looking down at your phone (as if you were always texting.) Overall, the biggest issue isn’t just how you look at your devices, but the amount of time you spend doing it. Keeping your neck in any position for hours without a break puts constant stress on your neck. And let’s be honest, most people don’t have the best posture while they scroll.
Usually, your shoulders are hunched, your head’s tilted down (anywhere from 45° to 60°), and all of your ligaments have to work overtime just to hold everything up. Normally, your neck can handle around 10lbs of force. But when you lean your head forward, suddenly you’re trying to manage up to 60lbs of force! After a while, that extra load really adds up.
Diagnosing
To diagnose text neck, your doctor will start with a physical exam. They’ll want to know what your normal routine looks like, especially how long and how often you use your devices. This helps them understand what your body goes through on a daily basis. They’ll also ask when your symptoms first started, what seems to make them worse, and how often you notice them.
From there, your doctor will feel around for any tender spots in your neck and shoulders. They’ll also guide you through different movements to look at your range of motion and pinpoint any possible triggers. But the most important thing they’ll do is a posture assessment to see if you have things like rounded shoulders or an excessive forward head tilt.
Treatment
Fixing text neck really comes down to 2 things: strengthening your neck and improving your posture. Luckily, physical therapy can help with both.
Your physical therapist will combine manual therapy techniques with targeted exercises to get your overworked muscles stronger and reduce the stress on your spine. They’ll also make some simple changes to help with your posture and protect your neck. One of the easiest (and most effective) things they’ll want you to make is raise your phone to eye level. Holding the screen up means you won’t have to constantly bend forward, which will do wonders for your neck. If you need to, invest in a phone case (like LoopyCases) that makes holding your phone up easier.
Whiplash
One of the more intense injuries you might experience is whiplash. Whiplash happens when your head is suddenly thrown forward and backward, like the snap of a whip. Such a rapid, forceful (and often unexpected) motion can stretch and even tear the ligaments in your neck.
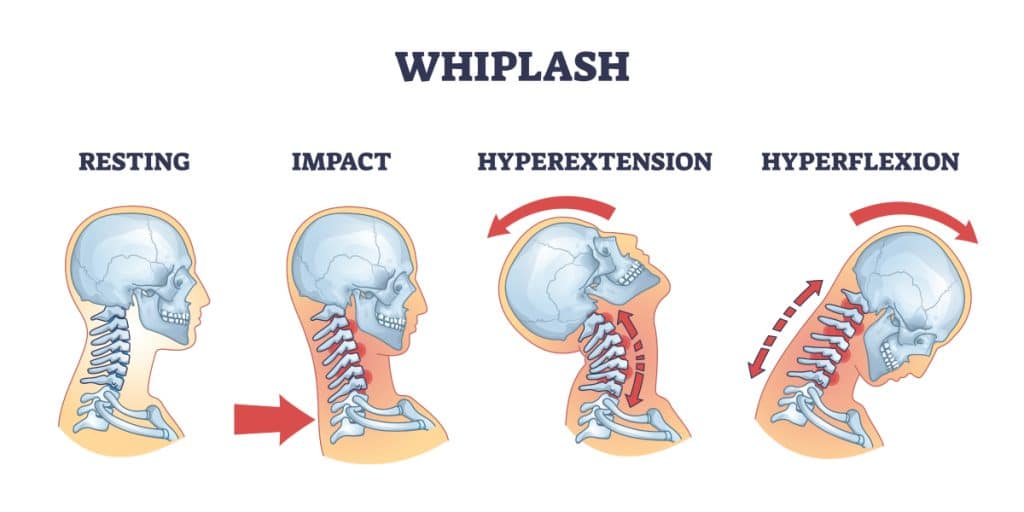
Most people picture car accidents or those crash test dummies when they think of whiplash. While it’s true that those types of collisions are one of the leading causes, there are other ways to get whiplash too. But more on that in a minute.
Symptoms
Whiplash doesn’t look exactly the same for everyone. Some symptoms can appear right away, while other symptoms may take several hours or days to develop. The severity of your injury usually determines how intense it all feels.
Since whiplash can be pretty violent, neck pain and stiffness are almost a guarantee, especially when you try to move. Don’t be surprised if you feel it in your shoulders and upper back too. Just turning and tilting your head will seem difficult.
Headaches are also very common. Typically, they start right at the base of your skull and shoot up toward the top of your head. Some people even get dizzy or have trouble concentrating. If your nerves are involved, then you might notice numbness or tingling down into your arms and hands.
Grades Of Whiplash
Whiplash ranges quite a bit in severity, so it’s graded on a scale from 0 to 4.
- Grade 0. You don’t have any symptoms or physical signs of injury, even after a few days.
- Grade 1. There’s minor pain and stiffness in your neck, but no other signs of injury.
- Grade 2. You still have pain and stiffness, but your range of motion is also restricted. This is the most common grade of whiplash.
- Grade 3. Similar to grade 2, but with neurological symptoms like numbness, tingling, or abnormal reflexes.
- Grade 4. The most severe, usually involving things like spinal instability, fractures, or serious nerve issues. You should get medical attention immediately.
Knowing the grade of whiplash helps determine the safest and most effective treatment plan.
Causes
Whiplash happens when your neck moves faster than your body can actually handle safely. Car accidents are a classic example, especially if you’re rear-ended. When you get hit from behind, your body gets pushed forward while your head is a second or 2 behind, creating a whip like motion.
It doesn’t stop there though. Contact sports like hockey, football, and rugby can cause similar forces from sudden hits. The same goes for rollercoasters. All that rapid acceleration and deceleration can put an extreme amount of force on your neck, especially if your head isn’t supported that well.
Age can also play a role. Adults 65 and older tend to get more severe cases of whiplash because their bones and ligaments aren’t as strong or flexible. Your body just isn’t able to absorb those sudden brutal forces very well, so your chances of getting injured are higher.
Diagnosing
Since there isn’t a special test that can diagnose whiplash, your doctor will have to focus on ruling out other serious conditions. First and foremost, they’ll want to know if you’ve been in any accidents or situations where your neck jerked back and forth. Then they’ll examine your posture, check your range of motion, and feel around your neck and upper back. If your symptoms are bad enough or involve neurological signs, they may order an MRI or X-ray to get the whole picture.
Treatment
Once you’re diagnosed, you’ll want to look for treatment that focuses on conservative, movement based care. As you can guess, that’s where physical therapy really shines. PT is such an effective way to treat whiplash because it helps you heal and manage your symptoms at the same time.
In the beginning, the main goal is to reduce your pain and gently restore movement. You’ll start with light range of motion exercises and hands-on techniques to ease the tension in your muscles and improve joint mobility. As you heal, you’ll progress to more strengthening and stability exercises for your neck, shoulders and upper back. Your therapist will also work with you to retrain your posture so your spine isn’t constantly strained.
Most people recover extremely well from whiplash, especially if they start physical therapy early. The key is to stay active (within safe limits), avoid overdoing it, and give your body the support it needs to heal. Before you know it, your symptoms will be gone and you’ll be back to doing the things you love.
Bones
As a quick recap, your neck is made up of seven bones, C1-C7, stacked neatly on top of each other.
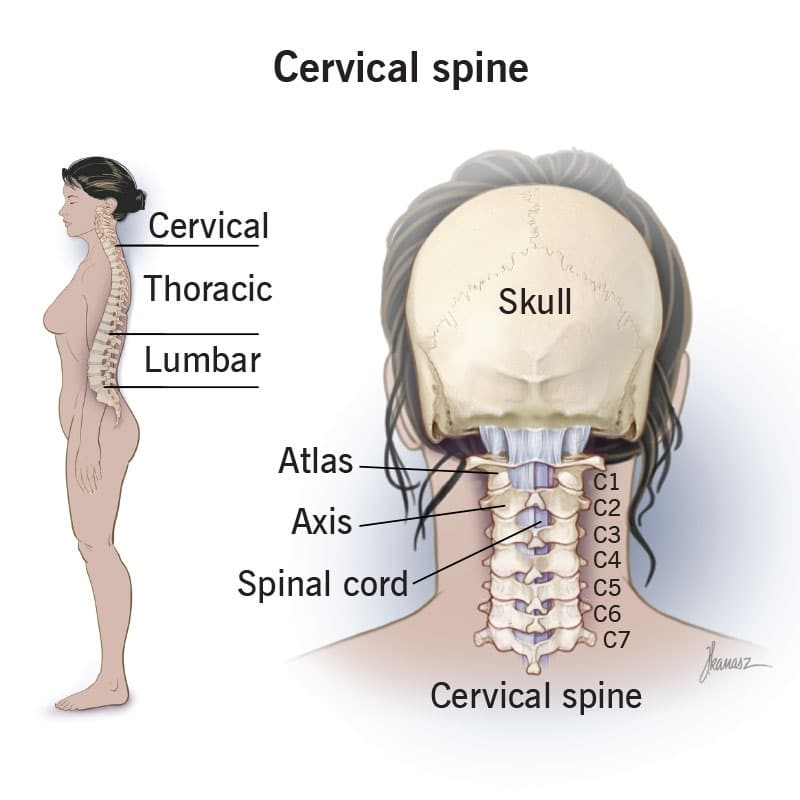
While they’re all important, 2 of the bones deserve their moment in the spotlight. At the very top sits C1, also known as the atlas. Unlike the other bones, it’s shaped like a ring and doesn’t have a typical vertebral “body”. Its main job is to help you move your head up and down, like you’re nodding “yes”.
Right below the atlas is C2, the axis. This one has a unique feature, small bony projections called dens. Basically, it acts as a pivot point (think Ross from Friends) so your head can rotate from side to side, like you’re shaking your head “no”.
Between the atlas, axis, the rest of your neck bones are intervertebral discs. These discs are made of specialized cartilage and act as a cushion for your spine. They also prevent your bones from grinding against each other so your neck can move smoothly.
Cervical DDD
The first injury we’re going to look at is cervical degenerative disc disease, or DDD. When you have cervical DDD, it means the discs in your neck are wearing down. As you get older, those discs naturally lose water, flexibility, and height. It’s just part of aging.
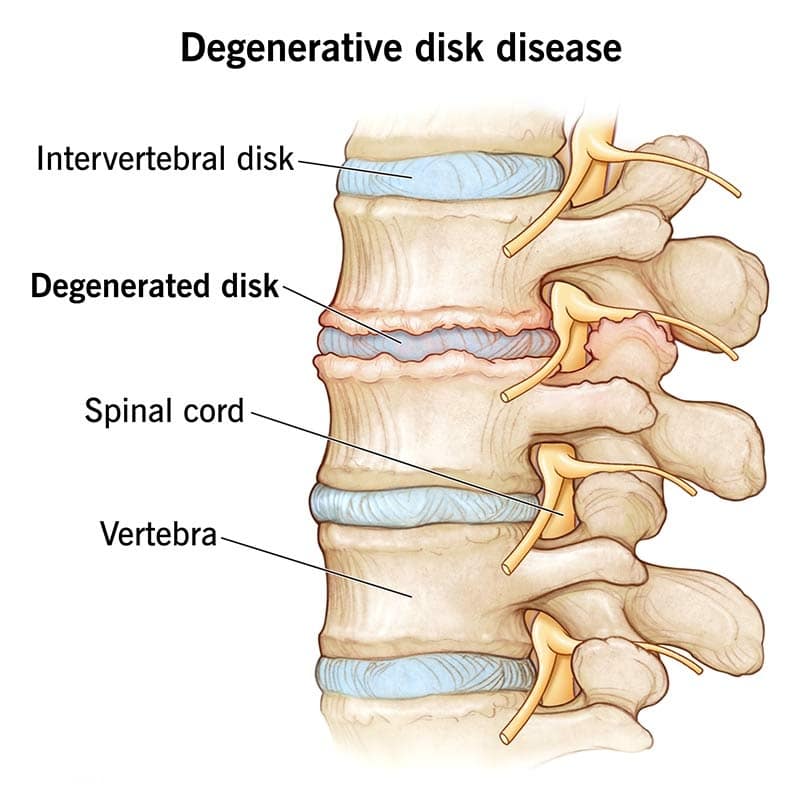
The problem is what happens next. Once your discs wear down enough, there’s nothing to stop your bones from rubbing together. This is what’s often called “bone on bone.” You’ve probably heard people talk about it in regards to their knees or back, but it can happen to your neck too. And not only is it incredibly painful, but it can also lead to other complications.
Symptoms
Here’s a fun (or not so fun) fact: most people over the age of 40 have at least a little bit of cervical DDD, even if they don’t feel it.
When symptoms do show up, pain is usually the first one you’ll experience. It might come and go, or stay for weeks at a time (sometimes longer). Certain movements and even just being in the same position for too long can make it worse. The pain may even travel into your shoulders, arms, and hands.
You might also notice some stiffness, muscle weakness, and limited range of motion in your neck as well. And don’t forget about headaches. Those are common too, especially right at the base of your skull.
Causes
Aging is the biggest one to blame here, but there are some things that can speed up the process. Obesity, traumatic injuries (such as a fall), and physically demanding jobs all increase your risk of cervical DDD. Women also tend to experience symptoms more than men.
Diagnosing
In order to diagnose cervical DDD, your doctor will start with an exam to check your strength, nerve function, and pain levels. From there, they’ll order an MRI or X-ray. These tests will give them a better look at your discs and how well they’re aligned.
DDD tends to progress in stages, so your doctor will want to figure out which one you fall into.
- Dysfunction. There’s early signs of wear and tear, and your symptoms are pretty mild.
- Dehydration. This is when your discs are starting to dry out and lose their height and flexibility. Symptoms usually get worse here too.
- Stabilization. At this stage, your spine is frantically trying to stabilize itself, which can be extremely painful and even cause spinal stenosis (you’ll learn about that in a bit.)
- Collapse. Your discs have shrunk so much that your bones are now rubbing together and possibly pressing against your nerves too, which can cause severe radiating pain.
Treatment
While you can’t reverse cervical DDD, physical therapy helps you manage it so you can still live comfortably. Physical therapy focuses on reducing the stress on your spine, improving movement, and strengthening the muscles that support your neck. Instead of just masking your symptoms, it tackles the root of your problem.
In the beginning, you’ll learn stretches and strengthening exercises that target specific muscles in your neck and shoulders. Tight muscles can limit your range of motion and make your pain worse, so improving flexibility is key. As you progress, the therapist will add new, more challenging exercises to restore your strength and stability.
Another important part of the puzzle is correcting your posture. Having poor posture, especially a forward head position, puts a ton of pressure on your cervical discs. Pt will help retrain how you stand, sit, and move throughout your day so it’s easy to stay in alignment. All in all, with the right combination of exercises, movement, and education, you’ll have fewer flare ups and improve your quality of life without invasive treatments (like surgery or injections.)
Cervical Spinal Stenosis
Next up is cervical spinal stenosis.
Think of your spine like a long tunnel made of bones stacked together. Running right through the middle of that tunnel is your spinal cord, which sends messages from your brain to the rest of your body. Now, imagine that tunnel slowly narrowing over time. That’s spinal stenosis.
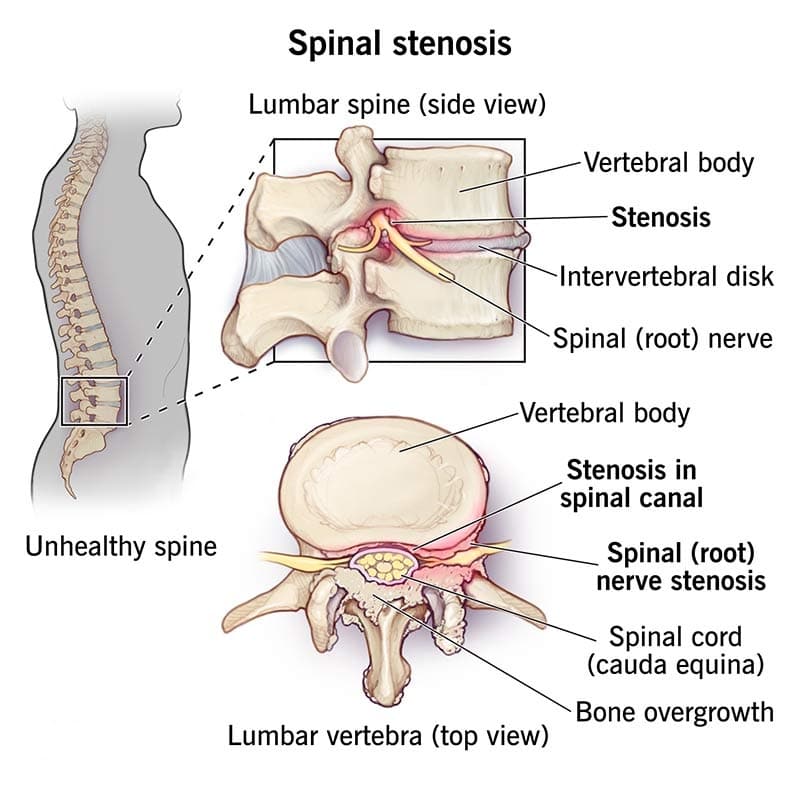
Symptoms
Spinal stenosis can be sneaky because it develops gradually, so you might not feel anything at first and then all of a sudden symptoms appear out of nowhere.
When it comes to pain, everyone experiences it a little differently. Some describe it as a deep bruise, while others feel more of a sharp, electric, burning sensation. It tends to come and go- flaring up, calming down, then returning again later on. If your nerves get involved, then you might have some numbness and tingling in your arms and hands.
Causes
It’s possible to be born with spinal stenosis, but it’s pretty rare (only about 9% of cases.) Most of the time, it’s something that you develop later on from aging and everyday wear and tear.
Certain conditions can speed up the process. For example, osteoarthritis slowly wears down the protective cartilage in your joints. When this happens, your body starts to grow bone spurs. These extra bits of bone can extend into your spinal canal and crowds your nerves.
Herniated or bulging discs also play a role. As you get older, the cushiony discs between your vertebra can dry out, flatten, or crack. Then that soft gel in the center leaks out and starts crowding your spinal cord and nerves, adding to that narrowing effect.
Diagnosing
To diagnose cervical spinal stenosis, your doctor will do the basics: review your medical history, ask about your symptoms, and do a physical exam. They might have you move your neck in different directions or apply pressure to see what exactly triggers your symptoms. Imaging, like an MRI or X-ray, usually comes next. This helps give the doctor a better idea of how much narrowing is going on inside your spine and what’s causing it.
Treatment
The good news is, most people don’t need surgery to treat cervical stenosis. It’ll all depend on how severe your symptoms are and what exactly is causing the narrowing in the first place. For more mild cases, basic things like ice or heat can help calm everything down.
If your symptoms seem to be sticking around, your doctor may recommend some anti-inflammatories or steroid injections. They’ll also want you to start physical therapy too.
While you can’t reverse the narrowing itself, physical therapy can make a big difference in how you feel. You’ll learn how to strengthen your neck and even different strategies that can relieve nerve pressure by slightly opening your spinal canal. At the end of the day, their goal is actually quite simple. They want to keep moving, reduce overall irritation, and help you manage your symptoms so they don’t take over your life.
Cervical Facet Joint Strain
Usually, people blame neck pain on poor posture or possibly a “slipped” disc. But more often than not, the real troublemaker is something much smaller: your facet joints.
These little joints sit along the back of your neck (cervical spine) and quietly work to keep your head stable and moving smoothly. When they get irritated, worn down, or inflamed, then you have what’s called cervical facet joint strain (CFJS.)
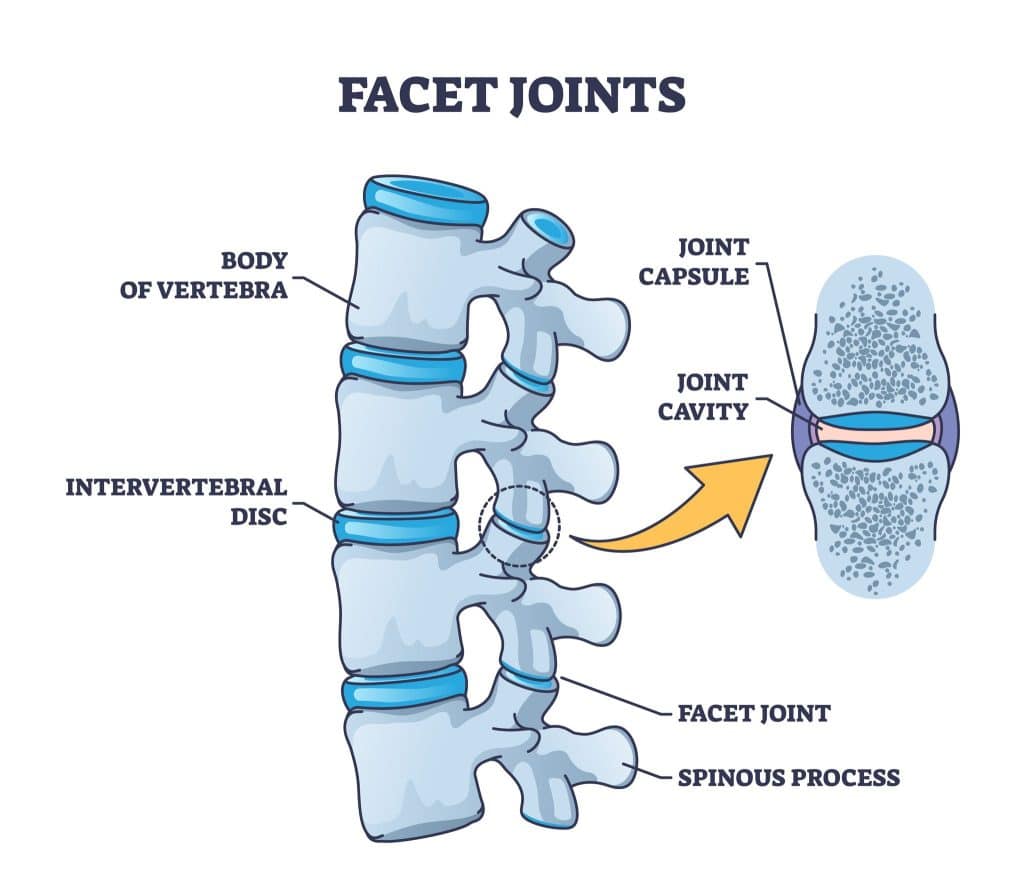
Symptoms
Like a lot of the neck injuries we’ve covered, people experience CFJS in different ways. It depends on how irritated the joint is and where the strain is located.
At first, you’ll probably notice some mild discomfort that comes and goes sporadically. It’s easy to brush off in the beginning. Manageable, annoying, but not a big deal. That is, until it starts showing up more frequently and more intense each time.
In most cases, the pain shows up right near the irritated joint. But your neck doesn’t work alone, it’s connected to your shoulders, upper back, and arms, so that pain can easily spread. You might also notice muscle spasms or some tingling “pins and needles” type sensation as well.
Causes
CFJS rarely comes from just one single thing. It’s actually a combination of factors that slowly add up over time.
Your facet joints are constantly moving and stabilizing, which makes them vulnerable. When something does go wrong, one of two things can happen: either the joint becomes too loose and unstable, or too stiff and restricted.
In most cases, wear and tear is to blame. Degenerative conditions, like facet joint degeneration, degenerative disc disease, or osteoarthritis gradually break down the cartilage in your joints. As that protective layer wears away, your joints take on more and more stress. In order to compensate, your body forms bone spurs, which end up irritating the joint (and nearby nerves) even more.
Certain injuries have been known to speed up CFJS. A car accident or big fall can force your neck beyond its limits, which stretches and even tears the ligaments around the joint. This can lead to hypermobility, which is just a fancy way of saying that your joint moves way more than it should.
And then there’s posture. Spending hours hunched over your phone or laptop puts a ton of extra strain on your neck. When you lose that natural curvature, your facet joints have to pick up the slack and absorb more stress than they’re meant to handle.
Diagnosing
Diagnosing CFJS starts with a physical exam from your doctor. They’ll ask about your symptoms, how long you’ve had them, and what seems to make them worse. Then they’ll watch how your neck moves to help determine which joint is causing the issue. This helps them figure out if the joint’s unstable, restricted, or just stiff.
Typically, imaging isn’t necessary, but your doctor may order some tests to rule out other conditions.
Treatment
Recovery from CFJS starts with understanding what exactly is going on with your neck. Knowing what triggers your symptoms and how to manage them will play a huge part in your recovery. And the best way to fully grasp everything is through physical therapy.
At first, your therapist will work on calming things down so you’re able to move without constantly being in pain. They’ll use soft tissue techniques to relax tight muscles and reduce spasms around your neck.
Once your pain improves, the real work begins.
The physical therapist will create an exercise program designed to restore movement back into your neck and make it stronger. Weak and imbalanced muscles can make facet joint problems worse, which is why you need to strengthen the deep stabilizing muscles in your neck and shoulders. Stronger support means less stress on your irritated facet joints.
The final part of treatment will focus on correcting your posture and returning to daily activities. Essentially, your goal isn’t just about feeling better, it’s about moving better too. You’ll learn how to do your normal everyday tasks safely without putting your neck into those stressful positions again.
All in all, recovery can take anywhere from a few weeks to a few months. It all comes down to consistency and how well you follow your treatment plan.
Cervical Fracture
One of the more serious neck injuries you can experience is a broken neck (also known as a cervical fracture.) Your neck is made up of 7 small bones, all of which have the ability to break. The bigger concern is your spinal cord, which runs right through the middle of them. So, even a tiny fracture is extremely serious.
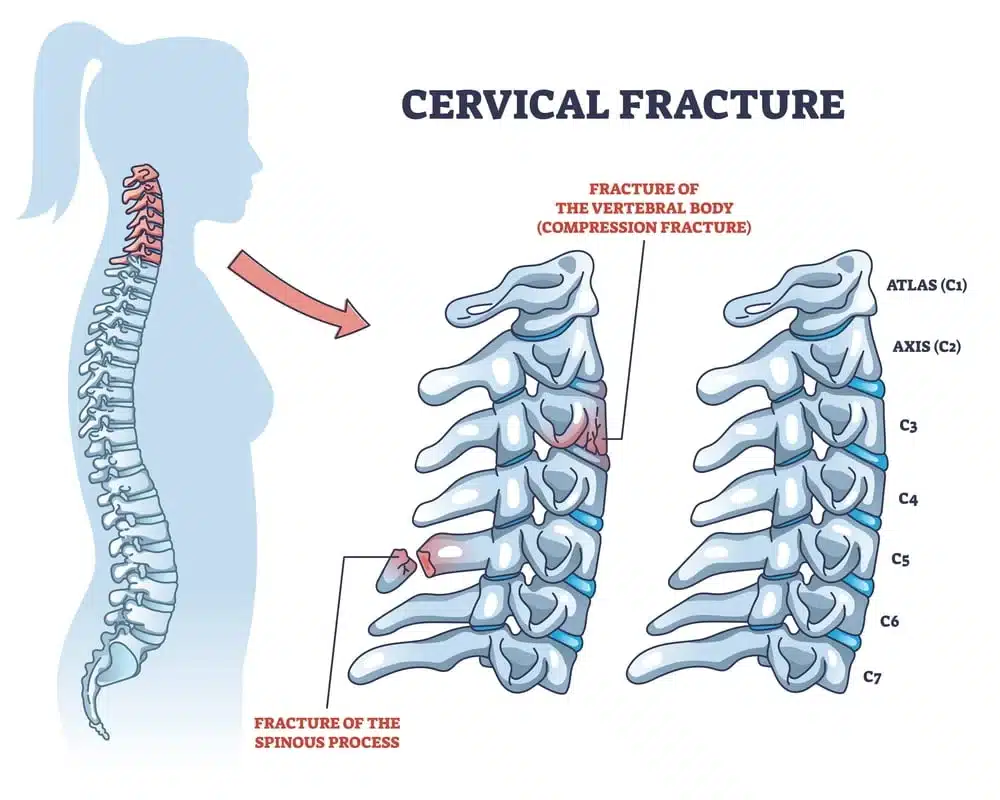
Symptoms
A couple of things come into play when you have a broken neck. You’ll experience different symptoms depending on the severity of the break and whether your spinal cord is involved.
Pain is almost always guaranteed. It can range anywhere from a dull ache to sharp and intense. Don’t be surprised if it also spreads into your shoulders and arms.
It actually takes quite a bit of force to break your neck, so there’s often visible signs too, like bruising, swelling, and tenderness. If your nerves are affected, then things start to escalate. You’ll get numbness, tingling, and even lose sensation in your arms. In more severe cases, paralysis can happen.
Causes
Most cervical fractures are caused by some sort of high impact situation, such as a car accident or major fall. These kinds of injuries involve a sudden, overwhelming force on your neck that your body just can’t handle.
Older adults face a different risk altogether. As your bones weaken with age, especially from certain conditions like osteoporosis, even minor falls can cause a fracture. Something as simple as tripping or slipping off a chair is all it takes.
Athletes are at a higher risk too, especially with fast-paced contact sports. Hockey players can get hit from behind and crash into the boards. Football players may lead with their head when they make a tackle. Even gymnasts might miss grabbing the bar and land wrong. All of these situations put a huge sudden force on your neck without any warning.
Diagnosing
It’s important to be cautious with all spinal injuries, especially if you think you’ve broken your neck. That’s why you always see doctors on TV immediately put people in a neck brace, to help prevent further damage. From there, they’ll do imaging. First, an X-ray, followed by an MRI or CT scan for a more detailed look at your bones.
Once the imaging is done, your doctor will do a neurological exam to check your nerve function. That means testing your strength, sensation, and reflexes, all to see whether your spinal cord has been affected.
Treatment
Treatment will depend on two things: which bone is broken and whether your nerves or spinal cord is involved. Typically, minor fractures just need a rigid neck brace. It usually takes about 8 to 12 weeks for the bone to heal. More complex or unstable breaks may require surgery to stabilize your spine before your healing journey can begin.
Once your bone heals, you’ll want to work on getting the strength and mobility back in your neck. The most effective (and safest) way to do this is with physical therapy. The therapist will guide you through a program that gradually (and safely) rebuilds the strength in your neck, shoulders, and upper back. You’ll also work on improving your posture and learning how to move in ways that protect your neck.
Cervical Spondylosis
This last injury, called cervical spondylosis, is what happens when years of wear and tear finally catch up with your neck. Think about it, your neck has a ton of responsibilities and rarely gets a break. It holds your head up, lets you turn and look around, and supports almost every movement you make on a daily basis. Over time, all that work really takes a toll. And eventually, that toll comes in the form of cervical spondylosis.
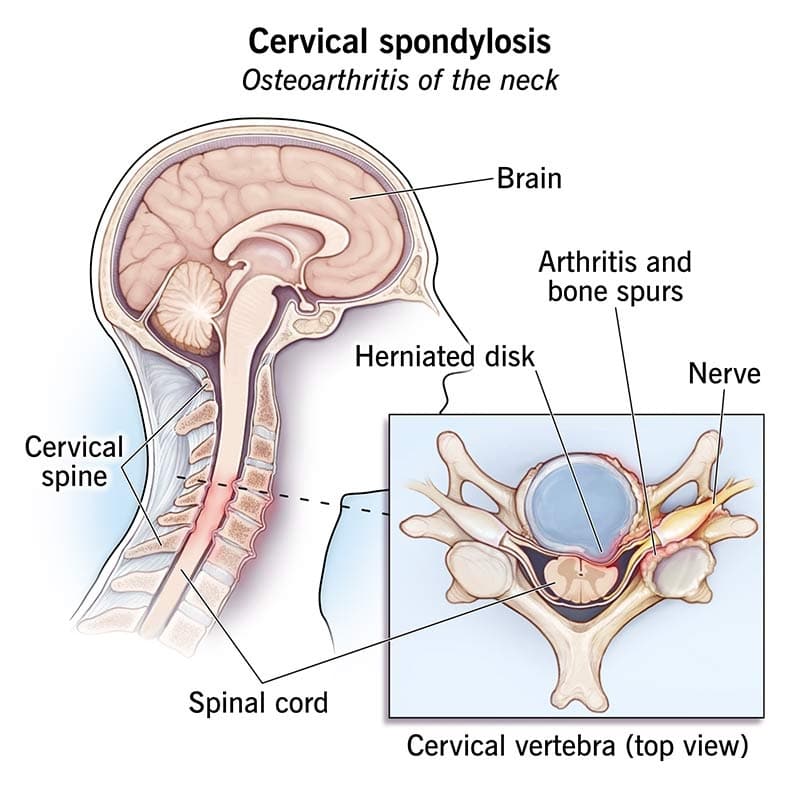
Spondylosis is just the technical way of saying arthritis. So cervical spondylosis simply means arthritis in your neck. It develops when the discs between your vertebrae slowly wear down. As your body tries to compensate, it forms bone spurs in an attempt to stabilize your spine. More on that in a minute though.
Symptoms
There aren’t always super obvious signs when you have cervical spondylosis. At first, it might feel like your usual aches and pains. You just brush it off and keep going with your day. But after a while, your symptoms will get worse and get harder to ignore.
Pain and stiffness are usually the first to show up. Most of the time it sticks to the neck area, but the discomfort can spread into your shoulders and upper back too. You might also notice a grinding or popping sound when you try to move your neck. Turning your neck can start to feel difficult from how tight everything is. Muscle spasms can creep in too, which might end up causing headaches near the base of your skull.
If the spondylosis compresses or irritates your nerves, then there might be some other symptoms to look out for. Pain might not stop at your shoulders, and you could get numbness, tingling, and even weakness in your arms.
Causes
So what exactly causes cervical spondylosis? Well, that’s simple: aging. As you get older all the structures in your neck naturally change. Your discs lose their moisture, height and flexibility. Unfortunately, this makes them less effective at their job (supporting your spine.) Once that protective layer breaks down, your joints are more exposed and can start developing arthritis.
Age isn’t the only factor though. Things like repeated strain can actually speed up the arthritis. Jobs or daily tasks around the house that constantly stress your neck add up over time. The same goes for spending hours hunched over your phone or tablet. That poor posture is quietly accelerating the wear and tear. Previous neck injuries also increase your odds, making your joints more vulnerable down the line.
Diagnosing
Diagnosing cervical spondylosis usually starts with getting a thorough medical history and then a physical exam. Since there aren’t any visible signs to tip them off, your doctor will ask you about your symptoms and check how your neck moves. Then they’ll test your strength and nerve function in your arms and hands to see if your nerves are involved.
To confirm their diagnosis, they’ll likely order an X-ray or MRI. These tests give a clear look at the changes in your spine and will also help rule out any other conditions that could be causing your neck pain.
Treatment
With the help of physical therapy, most people with cervical spondylosis can still have a full, active life without needing surgery. Your therapist will teach you how to reduce your pain, get more movement in your neck, and most importantly, protect your spine from further stress. You’ll learn exercises that you can do long after you graduate from PT, especially on days you start to feel some symptoms creep back in.
The other key thing they’ll do is tweak some of your daily habits. Things like fixing your posture, improving your workstation setup, and adjusting how you do certain tasks and activities will really help protect your neck. These changes might seem small, but they’ll make a huge difference. Before you know it, you’ll be moving better, hurting less, and getting back to the things you actually love.
To learn more about back and hip pain, click here.